Beckwith-Wiedemann Syndrome
Also known as: BWS
What is Beckwith-Wiedemann Syndrome?
Beckwith-Wiedemann syndrome was first described by doctors Bruce Beckwith and Hans Rudolph Wiedemann in the 1960’s. The doctors identified children who had a number of symptoms including body overgrowth, external intestines, enlarged tongues, and low blood sugar. When a child exhibited all of these characteristics, they described them as having Beckwith-Wiedemann syndrome. Today, approximately 1 in 13,700 people have the condition.
What are the clinical characteristics of BWS?
- Macroglossia (large tongue)
- Macrosomia (large body size) and/or hemihypertrophy (one side of body is bigger than the other side)
- Neonatal hypoglycemia (low blood sugar as newborn babies)
- Increased risk for certain types of tumors such as Wilm's tumor (kidney tumor) and hepatoblastoma (liver tumor)
- Omphalocele (born with intestines on the outside of the body) or umbilical hernia
- Creases or pits on the ears
- Normal intelligence
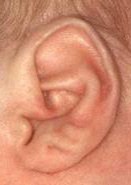
example of creases on ear

baby with enlarged tongue
What causes Beckwith-Wiedemann in children?
Beckwith-Wiedemann is a result of abnormal activity in the genes that regulate the body’s cell growth. While there is no single cause for the change of these genes, a geneticist can determine the source with special testing and evaluation. Most individuals with Beckwith-Wiedemann are the first affected in the family and the risk for recurrence is low. However, there may be a hereditary connection depending on the underlying cause.
What is the prognosis for my child with Beckwith-Wiedemann?
The prognosis for most children with this condition is generally positive, and treatment varies by child. It is important to monitor your child’s tumor development, but most children with Beckwith-Wiedemann will attend school, have friends, and enjoy life. With close follow-up by the craniofacial team and/or clinical geneticists at Nicklaus Children’s Hospital, your child can grow to become a healthy and happy adult.
Reviewed by: Chad Perlyn, MD
This page was last updated on: June 02, 2025 11:32 AM
Related Videos
Dr. Chad Perlyn is a pediatric plastic surgeon with the Division of Plastic Surgery at Nicklaus Children's Hospital. For more information, please visit nicklauschildrens.org/BWS

Inspiring Patient Stories

Their Medical Mystery Solved, a Family Helps Create Awareness of Beckwith-Wiedemann Syndrome
Crystal grew up believing that she was somehow “different” from other people. It wasn’t until the birth of her second child in 2017 that the Florida gulf coast mother of three found answers to personal mysteries she had pondered throughout her life.
Read More.
Learn more about
Hemihyperplasia
When one side of the body, such as the legs, arms, face or some combination of these, grows more than the other, this is known as hemihyperplasia.
Hepatoblastoma
A hepatoblastoma is a rare tumor that grows from the cells of the liver.
Macroglossia
Macroglossia is the medical term for when a child is born with an enlarged tongue. It is one of the most common features of Beckwith-Wiedemann Syndrome.
Gastroschisis and Omphalocele
Gastroschisis and omphalocele are both part of a relatively uncommon group of birth defects that involve an opening or hole in the abdominal wall, frequently on the right side of the belly button.
Pinna Abnormalities & Low-Set Ears
The pinna is another term for the outer ear. When abnormalities occur with the shape or location of the ears when the baby is still growing in the womb, this may be the sign of certain medical conditions.
Macroglossia Surgery
Macroglossia is the medical term for an abnormally large tongue that is present at birth. In some cases, surgery is required to treat the problem and help the child eat, breathe, and speak more easily.